Healthcare
The right to health is a basic human right embodied in various international legal constitutions. This right includes, not only, access to a healthcare system, but also access to other determinants of health – nutrition, water and sanitation, housing, safe environmental conditions, health-related education, non-discrimination and life in human dignity.
Health impacts of disasters:
- Direct: injury, physiological trauma
- Indirect: increased rates of infectious diseases, malnutrtion, complications of chronic diseases.
These impacts are related to factors such as: inadequate quantity and quality of water, breakdown of sanitation, food shortage, disruption oh health service, overcrowding and population displacements. Therefore, health relief efforts should be addressed in cooperation and coordination with any other relief efforts / sectors, whether regarding food, settlement etc., and should be implemented according to the same principles guiding any relief work.
Primary goals of humanitarian response/ disaster healthcare:
- Prevent and reduce excess mortality, early interventions, focus on immediate survival needs.
- Meet the most important needs, appropriate coverage, accessibility, promotion of quality.
Mortality
- Causes of mortality are identified, documented and monitored.
- Maintain or reduce a mortality rate of less than twice the baseline rate prior to the disaster.
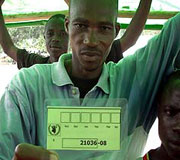 Installment and coordination
Installment and coordination
- An initial assessment in cooperation with local authorities and population is taken about the affected population and demography, the disaster affected area, existing health structures, the effects of the disaster onto those, and available resources of staff, skills, medication, equipment, facilities, logistics, infrastructure and information systems.
- If possible in cooperation with the local ministry of health, otherwise the UN/ WHO, or locally active NGOs.
- In cooperation with the health authority a strategy is planned, to ensure integration of local facilities and sustainability of the program. The strategy is built on existing systems and integrates capacities.
- Priority is to support and strengthen local health facilities and to integrate local health staff. Attention is paid to gender and ethnic balance, while respecting cultural conditions.
- Coordination mechanisms for the activities of different organizations are installed and monitored by regular meetings.
- If existing, local national health guidelines are regarded.
- Participation of the affected population is important to develop recovery and resistance capacities for future disasters, to aim at the sustainability of the healthcare system and to not undermine existing structures.
- Assure coverage and accessibility of priority health interventions, for all members of the community, ensure equity, including the most vulnerable groups and their needs (women, children, elderly, HIV/AIDS infected). In practice this is implemented in the location and staffing of the health service, and if fees are charged, they are eliminated for those who can’t afford them.
- Adapt to local cultural habits.
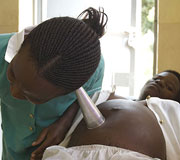
 Prevention and primary health care
Prevention and primary health care
- Intervention based on the priority of providing the most appropriate health benefit to the greatest number of people.
- Often that means the supply of the basic conditions that provide health: safe water, sanitation, food security, nutrition services, shelter and basic clinic care.
- All members of the community have access to health information: about behavior that protects and promotes good health, about major health risks and endemic health problems and about the availability and location of health services.
- People are encouraged to seek early care for fever, cough, diarrhea.
- Clinical services should primarily aim to prevent and control diseases of epidemic potential e.g. by vaccination campaigns. Although hospital-based care is important, it usually has a smaller public health impact than primary health care interventions.
- Chronic diseases that have been treated before the disaster are continued to be treated according to their severity. If they haven’t been treated before, in a disaster priority is not given to staring a treatment.
- Vaccination campaigns; most often: measles for children, as they are most contagious: goal of vaccinating 95% of children 6 months to 15 years; although older children aren’t in danger of dying they can be affected as a disease transmitter, pertussis diphtheria.
- In case of a malaria or tuberculosis outbreak, drug treatment has to be chosen carefully after a survey according to drug resistance and handed out only structured and monitored, to avoid contributing to the spread of multi-drug resistant bacteria.
 Clinical Care
Clinical Care
- Goal: standardization of clinical services
- Health structure consists of a mixture of communal care of qualified health workers and birth attendants and central hospitals with doctors and inpatient care.
- Priority is to update existing local hospitals. Parallel health facilities, including field hospitals, are only installed if local facilities are exceeded or if certain population groups don’t have access. Field hospitals can be useful for the immediate care after a disaster, or while a hospital that has been destroyed is being reconstructed.
- Mobile clinics are only installed in consultation with local health authorities: They can fulfill a vital need to access remote communities, but if underutilized, or if they displace existing health services, they are a waste of limited resources.
- Number, level and location of health facilities and staffing should meet the demands of local population. The composition of the staff should also address minorities, eg. even one woman or ethnic minority worker increases the accessibility for those groups.
- Utilization rates are monitored: If utilization rates are below the average, it may indicate inadequate accessibility, if rates are above the average it may suggest a specific public health problem, or an under-estimation of the target population.
- Standardized case management protocols and drug lists should be established and handed over to health agencies, so that the appropriateness of standardizations can be controlled and adapted.
- A standardized essential drug list and management system ensures that people have consistent access and that drugs are used efficiently, rationally and cost-effectively.
- An appropriate number of birth delivery kits are available and are handed out to pregnant women and skilled/ traditional birth attendants.
- Health staff must be properly educated. If necessary, relief agencies provide training.
- The right of the patient to privacy, confidentiality and information about his condition and treatment are respected.
- Dead bodies are disposed off in a hygienic, dignified and culturally appropriate way. Unceremonious mass burials are to be avoided as they violate social norms and mostly can’t be defended as a public health measure. Only in few certain cases do human bodies pose a health risk if not buried immediately, eg. in case of death through cholera.

 Injuries
Injuries
- Even in disaster with a high number of injuries health care follows the principle of taking those measures that provide the greatest benefit to the highest number of people.
- Basic medical care and non-operative procedures can be life-saving even in severe injuries before surgery is implemented. eg. cleaning the airway, intravenous fluids, treatment of wounds. Therefore even in disasters with a large number of injuries priority is given to basic health care and in training local staff/ people to be able to provide initial treatment. Transferal points for first treatment, from which patients are transferred to clinics for surgery can be an efficient strategy. Bad surgery can be more harmful than no surgery at all.
- Triage means the categorization of patients according to their injury. Priority is not always given to the most severely injured, but to those where an operation has the greatest potential for being needed but for being successful in ensuring survival.
Outbreak preparedness
- Investigation and control plans and protocols are prepared and staff is trained.
- Reserve stocks of essential drugs and medicines, vaccines and basic protection material.
- Sources of vaccines procurement are identified for sudden rapid procurement for relevant diseases, eg. measles, yellow fever, meningitis..
- Sites for isolation and treatment of patients with endemic diseases are identified in advance, eg. for cholera camps.
- Sampling material transport media and a reference laboratory, whether local, national or international, for monitoring and ensuring diagnosis the development of the endemic is identified, and rapid test for on-site evaluation.
- If an indication of an outbreak is found, investigation occurs within 24 hours, math given with exact data of timer, place and person to identify high risk groups, and safety precautions are taken.
- For different diseases distinct frequency rates for indicating an endemic outbreak are defined, for eg. cholera one is enough, while for malaria a rate higher than the frequent rate of the season is needed.
- Sources of disease are controlled, eg. water quality.
- Other means of protection are activated, eg handing out mosquito nets and repellents in case of a malaria outbreak.